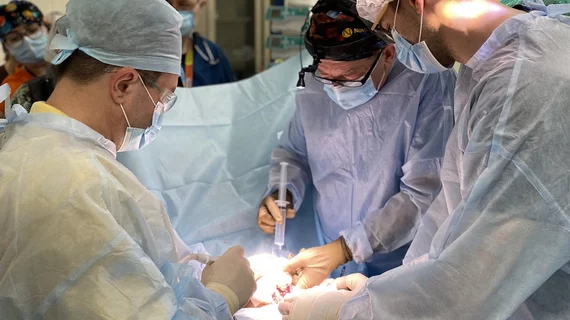
Americans more likely to seek surgical care during pandemic if hospital staff is vaccinated
A new study found Americans are more likely to have surgery during a pandemic such as COVID-19 if they are vaccinated, the hospital staff are vaccinated, the surgery is urgent and the surgery is an outpatient procedure. The study was published in the journal Vaccine.[1]
The study sheds additional light on what patients want regarding the recent debate about whether healthcare organizations should require clinicians to be vaccinated. Some healthcare systems do not require vaccines for COVID or the annual flu, while others have strict vaccination policies even prior to COVID. The study also reinforced the fact that patients want outpatient procedures to avoid overnight stays.
“It’s critical to understand what factors affect a patient’s decision to have surgery during an infectious pandemic if we want to help reduce deaths and illness. These factors include vaccination status of the patient and hospital staff, the need and length of hospital stay, and urgency of the procedure,” said Keith Ruskin, MD, FASA, study co-author, member of the American Society of Anesthesiologists (ASA) Committee on Patient Safety and Education and professor of anesthesia and critical care at the University of Chicago, in a statement. “Having this knowledge could help guide health care institutions’ future vaccine resource allocations and policies for vaccine requirements.”
The biggest impact on a patients’ willingness to have surgery during a pandemic was the urgency of surgery. Participants viewed life-saving surgery as more essential than an elective procedure like knee replacements during a pandemic.
The study also showed participants who were vaccinated were more willing to have a surgical procedure than their unvaccinated counterparts. Requiring hospital staff to be vaccinated also played a key role, with 24% of respondents saying they were unwilling to have lifesaving surgery without universal vaccination of hospital staff. This number decreased to 15% with universal vaccination, the authors note.
“Making the choice to not have surgery for an actual health problem could increase the risk of potential illness and disease attributable to pandemic-related fears,” explained Anna Clebone Ruskin, MD, study co-author and associate professor of anesthesia and critical care, University of Chicago, said in the statement. “This suggests a potential opportunity for public education.”
In the study conducted by the University of Chicago and Embry-Riddle Aeronautical University, 2,006 U.S. adults aged 18 or older were surveyed about a hypothetical surgery. They were recruited electronically using Amazon’s Mechanical Turk and answered a 26-item survey. Willingness to undergo surgery was assessed under several circumstances, including the urgency of surgery, time in the hospital, vaccination status of the participant, and if the hospital required all staff to be vaccinated. Data were collected in June 2021 amid the current SARS-CoV-2 pandemic.
Find more content on the impact of COVID-19 on healthcare
Reference: